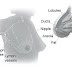
The Lungs
 Your lungs
are a pair of large organs in your chest. They are part of your
respiratory system. Air enters your body through your nose or mouth. It
passes through your windpipe (trachea) and through each bronchus, and
goes into your lungs. When you breathe in, your lungs expand with air.
Your lungs
are a pair of large organs in your chest. They are part of your
respiratory system. Air enters your body through your nose or mouth. It
passes through your windpipe (trachea) and through each bronchus, and
goes into your lungs. When you breathe in, your lungs expand with air.
This is how your body gets oxygen. When you breathe out, air goes out of your lungs. This is how your body gets rid of carbon dioxide. Your right lung has three parts (lobes). Your left lung is smaller and has two lobes. A thin tissue (the pleura) covers the lungs and lines the inside of the chest. Between the two layers of the pleura is a very small amount of fluid (pleural fluid). Normally, this fluid does not build up.
Cancer Cells
Cancer begins in cells, the building blocks that make up tissues. Tissues make up the organs of the body. Normal, healthy cells grow and divide to form new cells as the body needs them. When normal cells grow old or become damaged, they die, and new cells take their place. Sometimes, this orderly process goes wrong. New cells form when the body does not need them, and old or damaged cells do not die as they should. The build-up of extra cells often forms a mass of tissue called a growth or tumor.
Tumor cells can be benign (not cancer) or malignant (cancer). Benign tumor cells are usually not as harmful as malignant tumor cells:
Benign lung tumors :-
*are rarely a threat to life
*usually do not need to be removed
* do not invade the tissues around them
* do not spread to other parts of the body
Malignant lung tumors:-
*may be a threat to life
*may grow back after being removed
*can invade nearby tissues and organs
*can spread to other parts of the body Cancer cells spread by breaking away from the original tumor. They enter blood vessels or lymph vessels, which branch into all the tissues of the body. The cancer cells attach to other organs and form new tumors that may damage those organs. The spread of cancer is called metastasis.
Risk Factors
Doctors cannot always explain why one person develops lung cancer and another does not. However, we do know that a person with certain risk factors may be more likely than others to develop lung cancer. A risk factor is something that may increase the chance of developing a disease. Studies have found the following risk factors for lung cancer:
* Tobacco smoke:
Tobacco smoke causes most cases of lung cancer. It's by far the most important risk factor for lung cancer. Harmful substances in smoke damage lung cells. That's why smoking cigarettes, pipes, or cigars can cause lung cancer and why secondhand smoke can cause lung cancer in nonsmokers. The more a person is exposed to smoke, the greater the risk of lung cancer.
* Radon:
Radon is a radioactive gas that you cannot see, smell, or taste. It forms in soil and rocks. People who work in mines may be exposed to radon. In some parts of the country, radon is found in houses. Radon damages lung cells, and people exposed to radon are at increased risk of lung cancer. The risk of lung cancer from radon is even higher for smokers.
* Asbestos and other substances:
People who have certain jobs (such as those who work in the construction and chemical industries) have an increased risk of lung cancer. Exposure to asbestos, arsenic, chromium, nickel, soot, tar, and other substances can cause lung cancer. The risk is highest for those with years of exposure. The risk of lung cancer from these substances is even higher for smokers.
* Air pollution:
Air pollution may slightly increase the risk of lung cancer. The risk from air pollution is higher for smokers.
* Family history of lung cancer:
People with a father, mother, brother, or sister who had lung cancer may be at slightly increased risk of the disease, even if they don't smoke.
Screening
Screening tests may help doctors find and treat cancer early. They have been shown to be very helpful in some cancers such as breast cancer. Currently, there is no generally accepted screening test for lung cancer. Several methods of detecting lung cancer have been studied as possible screening tests. The methods under study include tests of sputum (mucus brought up from the lungs by coughing), chest x-rays, or spiral (helical) CT scans. You can read more about these tests in the Diagnosis section. However, screening tests have risks. For example, an abnormal x-ray result could lead to other procedures (such as surgery to check for cancer cells), but a person with an abnormal test result might not have lung cancer. Studies so far have not shown that screening tests lower the number of deaths from lung cancer. You may want to talk with your doctor about your own risk factors and the possible benefits and harms of being screened for lung cancer. Like many other medical decisions, the decision to be screened is a personal one. Your decision may be easier after learning the pros and cons of screening.
Symptoms
Early lung cancer often does not cause symptoms. But as the cancer grows, common symptoms may include:
* a cough that gets worse or does not go away
* breathing trouble, such as shortness of breath
* constant chest pain
* coughing up blood
* a hoarse voice
* frequent lung infections, such as pneumonia
* feeling very tired all the time
* weight loss with no known cause Most often these symptoms are not due to cancer. Other health problems can cause some of these symptoms. Anyone with such symptoms should see a doctor to be diagnosed and treated as early as possible.
Diagnosis
If you have a symptom that suggests lung cancer, your doctor must find out whether it's from cancer or something else. Your doctor may ask about your personal and family medical history. Your doctor may order blood tests, and you may have one or more of the following tests:
* Physical exam:
Your doctor checks for general signs of health, listens to your breathing, and checks for fluid in the lungs. Your doctor may feel for swollen lymph nodes and a swollen liver.
* Chest x-ray:
X-ray pictures of your chest may show tumors or abnormal fluid.
* CT scan:
Doctors often use CT scans to take pictures of tissue inside the chest. An x-ray machine linked to a computer takes several pictures. For a spiral CT scan, the CT scanner rotates around you as you lie on a table. The table passes through the center of the scanner. The pictures may show a tumor, abnormal fluid, or swollen lymph nodes. Finding Lung Cancer Cells The only sure way to know if lung cancer is present is for a pathologist to check samples of cells or tissue. The pathologist studies the sample under a microscope and performs other tests. There are many ways to collect samples. Your doctor may order one or more of the following tests to collect samples
* Thoracentesis:
The doctor uses a long needle to remove fluid (pleural fluid) from the chest. The lab checks the fluid for cancer cells.
* Bronchoscopy:
The doctor inserts a thin, lighted tube (a bronchoscope) through the nose or mouth into the lung. This allows an exam of the lungs and the air passages that lead to them. The doctor may take a sample of cells with a needle, brush, or other tool. The doctor also may wash the area with water to collect cells in the water.
* Fine-needle aspiration:
The doctor uses a thin needle to remove tissue or fluid from the lung or lymph node. Sometimes the doctor uses a CT scan or other imaging method to guide the needle to a lung tumor or lymph node.
* Thoracoscopy:
The surgeon makes several small incisions in your chest and back. The surgeon looks at the lungs and nearby tissues with a thin, lighted tube. If an abnormal area is seen, a biopsy to check for cancer cells may be needed.
* Thoracotomy:
The surgeon opens the chest with a long incision. Lymph nodes and other tissue may be removed.
* Mediastinoscopy:
The surgeon makes an incision at the top of the breastbone. A thin, lighted tube is used to see inside the chest. The surgeon may take tissue and lymph node samples.
You may want to ask these questions before the doctor takes a sample of tissue:
* Which procedure do you recommend? How will the tissue be removed?
* Will I have to stay in the hospital? If so, for how long?
* Will I have to do anything to prepare for it?
* How long will it take? Will I be awake? Will it hurt?
* Are there any risks? What is the chance that the procedure will make my lung collapse? What are the chances of infection or bleeding after the procedure?
* How long will it take me to recover? * How soon will I know the results? Who will explain them to me?
* If I do have cancer, who will talk to me about next steps? When?
Types of Lung Cancer
The pathologist checks the sputum, pleural fluid, tissue, or other samples for cancer cells. If cancer is found, the pathologist reports the type. The types of lung cancer are treated differently. The most common types are named for how the lung cancer cells look under a microscope:
* Small cell lung cancer:
About 13 percent of lung cancers are small cell lung cancers. This type tends to spread quickly.
* Non-small cell lung cancer:
Most lung cancers (about 87 percent) are non-small cell lung cancers. This type spreads more slowly than small cell lung cancer.
Staging To plan the best treatment, your doctor needs to know the type of lung cancer and the extent (stage) of the disease. Staging is a careful attempt to find out whether the cancer has spread, and if so, to what parts of the body. Lung cancer spreads most often to the lymph nodes, brain, bones, liver, and adrenal glands. When cancer spreads from its original place to another part of the body, the new tumor has the same kind of cancer cells and the same name as the original cancer. For example, if lung cancer spreads to the liver, the cancer cells in the liver are actually lung cancer cells. The disease is metastatic lung cancer, not liver cancer. For that reason, it's treated as lung cancer, not liver cancer. Doctors call the new tumor "distant" or metastatic disease.
Staging may involve blood tests and other tests:
* CT scan:
CT scans may show cancer that has spread to your liver, adrenal glands, brain, or other organs. You may receive contrast material by mouth and by injection into your arm or hand. The contrast material helps these tissues show up more clearly. If a tumor shows up on the CT scan, your doctor may order a biopsy to look for lung cancer cells.
* Bone scan:
A bone scan may show cancer that has spread to your bones. You receive an injection of a small amount of a radioactive substance. It travels through your blood and collects in your bones. A machine called a scanner detects and measures the radiation. The scanner makes pictures of your bones on a computer screen or on film.
* MRI:
Your doctor may order MRI pictures of your brain, bones, or other tissues. MRI uses a powerful magnet linked to a computer. It makes detailed pictures of tissue on a computer screen or film.
* PET scan:
Your doctor uses a PET scan to find cancer that has spread. You receive an injection of a small amount of radioactive sugar. A machine makes computerized pictures of the sugar being used by cells in the body. Cancer cells use sugar faster than normal cells, and areas with cancer look brighter on the pictures. Stages of Small Cell Lung Cancer Doctors describe small cell lung cancer using two stages:
* Limited stage:
Cancer is found only in one lung and its nearby tissues.
* Occult stage:
Lung cancer cells are found in sputum or in a sample of water collected during bronchoscopy, but a tumor cannot be seen in the lung.
* Stage 0:
Cancer cells are found only in the innermost lining of the lung. The tumor has not grown through this lining. A Stage 0 tumor is also called carcinoma in situ. The tumor is not an invasive cancer.
* Stage IA:
The lung tumor is an invasive cancer. It has grown through the innermost lining of the lung into deeper lung tissue. The tumor is no more than 3 centimeters across (less than 1 ¼ inches). It is surrounded by normal tissue and the tumor does not invade the bronchus. Cancer cells are not found in nearby lymph nodes.
* Stage IB:
The tumor is larger or has grown deeper, but cancer cells are not found in nearby lymph nodes. The lung tumor is one of the following (see the picture of the main bronchus and pleura): -The tumor is more than 3 centimeters across. - It has grown into the main bronchus. - It has grown through the lung into the pleura.
* Stage IIA:
The lung tumor is no more than 3 centimeters across. Cancer cells are found in nearby lymph nodes.
* Stage IIB:
The tumor is one of the following:
-Cancer cells are not found in nearby lymph nodes, but the tumor has invaded the chest wall, diaphragm, pleura, main bronchus, or tissue that surrounds the heart
- Cancer cells are found in nearby lymph nodes, and one of the following:
*The tumor is more than 3 centimeters across
. * It has grown into the main bronchus.
* It has grown through the lung into the pleura.
* Stage IIIA:
The tumor may be any size. Cancer cells are found in the lymph nodes near the lungs and bronchi, and in the lymph nodes between the lungs but on the same side of the chest as the lung tumor.
* Stage IIIB:
The tumor may be any size. Cancer cells are found on the opposite side of the chest from the lung tumor or in the neck. The tumor may have invaded nearby organs, such as the heart, esophagus, or trachea. More than one malignant growth may be found within the same lobe of the lung. The doctor may find cancer cells in the pleural fluid.
Surgery and radiation therapy are local therapies. They remove or destroy cancer in the chest. When lung cancer has spread to other parts of the body, local therapy may be used to control the disease in those specific areas. For example, lung cancer that spreads to the brain may be controlled with radiation therapy to the head.
Second Opinion
Before starting treatment, you might want a second opinion about your diagnosis and treatment plan. Many insurance companies cover a second opinion if you or your doctor requests it. It may take some time and effort to gather your medical records and see another doctor. In most cases, a brief delay in starting treatment will not make treatment less effective. To make sure, you should discuss this delay with your doctor. Sometimes people with lung cancer need treatment right away. For example, a doctor may advise a person with small cell lung cancer not to delay treatment more than a week or two. There are many ways to find a doctor for a second opinion. You can ask your doctor, a local or state medical society, a nearby hospital, or a medical school for names of specialists. Also, your nearest cancer center can tell you about doctors who work there.
Comfort Care
Lung cancer and its treatment can lead to other health problems. You may need comfort care to prevent or control these problems. Comfort care is available both during and after treatment. It can improve your quality of life. Your health care team can tell you more about the following problems and how to control them:
* Pain:
Your doctor or a pain control specialist can suggest ways to relieve or reduce pain.
* Shortness of breath or trouble breathing:
People with lung cancer often have trouble breathing. Your doctor may refer you to a lung specialist or respiratory therapist. Some people are helped by oxygen therapy, photodynamic therapy, laser surgery, cryotherapy, or stents.
* Fluid in or around lungs:
Advanced cancer can cause fluid to collect in or around the lungs. The fluid can make it hard to breathe. Your health care team can remove fluid when it builds up. In some cases, a procedure can be done that may prevent fluid from building up again. Some people may need chest tubes to drain the fluid.
* Pneumonia:
You may have chest x-rays to check for lung infections. Your doctor can treat infections.
* Cancer that spreads to the brain:
Lung cancer can spread to the brain. The symptoms may include headache, seizures, trouble walking, and problems with balance. Medicine to relieve swelling, radiation therapy, or sometimes surgery can help. People with small cell lung cancer may receive radiation therapy to the brain to try to prevent brain tumors from forming. This is called prophylactic cranial irradiation
. * Cancer that spreads to the bone:
Lung cancer that spreads to the bone can be painful and can weaken bones. You can ask for pain medicine, and the doctor may suggest external radiation therapy. Your doctor also may give you drugs to help lower your risk of breaking a bone.
* Sadness and other feelings:
It's normal to feel sad, anxious, or confused after a diagnosis of a serious illness. Some people find it helpful to talk about their feelings.
Sources of Support
Learning you have lung cancer can change your life and the lives of those close to you. These changes can be hard to handle. It's normal for you, your family, and your friends to have many different and sometimes confusing feelings. You may worry about caring for your family, keeping your job, or continuing daily activities. Concerns about treatments and managing side effects, hospital stays, and medical bills are also common. Because most people who get lung cancer were smokers, you may feel like doctors and other people assume that you are or were a smoker (even if you weren't). You may feel as though you're responsible for getting cancer (or that others blame you). It's normal for anyone coping with a serious illness to feel fear, guilt, anger, or sadness. It may help to share your feelings with family, friends, a member of your health care team, or another person with cancer. Here's where you can go for support:
* Doctors, nurses, and other members of your health care team can answer many of your questions.
* Social workers, counselors, or members of the clergy can be helpful if you want to talk about your feelings or concerns. Often, social workers can suggest resources for financial aid, transportation, home care, or emotional support.
* Support groups also can help. In these groups, patients or their family members meet with other patients or their families to share what they have learned about coping with the disease and the effects of treatment. Groups may offer support in person, over the telephone, or on the Internet. You may want to talk with a member of your health care team about finding a support group.

This is how your body gets oxygen. When you breathe out, air goes out of your lungs. This is how your body gets rid of carbon dioxide. Your right lung has three parts (lobes). Your left lung is smaller and has two lobes. A thin tissue (the pleura) covers the lungs and lines the inside of the chest. Between the two layers of the pleura is a very small amount of fluid (pleural fluid). Normally, this fluid does not build up.
Cancer Cells
Cancer begins in cells, the building blocks that make up tissues. Tissues make up the organs of the body. Normal, healthy cells grow and divide to form new cells as the body needs them. When normal cells grow old or become damaged, they die, and new cells take their place. Sometimes, this orderly process goes wrong. New cells form when the body does not need them, and old or damaged cells do not die as they should. The build-up of extra cells often forms a mass of tissue called a growth or tumor.
Tumor cells can be benign (not cancer) or malignant (cancer). Benign tumor cells are usually not as harmful as malignant tumor cells:
Benign lung tumors :-
*are rarely a threat to life
*usually do not need to be removed
* do not invade the tissues around them
* do not spread to other parts of the body
Malignant lung tumors:-
*may be a threat to life
*may grow back after being removed
*can invade nearby tissues and organs
*can spread to other parts of the body Cancer cells spread by breaking away from the original tumor. They enter blood vessels or lymph vessels, which branch into all the tissues of the body. The cancer cells attach to other organs and form new tumors that may damage those organs. The spread of cancer is called metastasis.
Risk Factors
Doctors cannot always explain why one person develops lung cancer and another does not. However, we do know that a person with certain risk factors may be more likely than others to develop lung cancer. A risk factor is something that may increase the chance of developing a disease. Studies have found the following risk factors for lung cancer:
* Tobacco smoke:
Tobacco smoke causes most cases of lung cancer. It's by far the most important risk factor for lung cancer. Harmful substances in smoke damage lung cells. That's why smoking cigarettes, pipes, or cigars can cause lung cancer and why secondhand smoke can cause lung cancer in nonsmokers. The more a person is exposed to smoke, the greater the risk of lung cancer.
* Radon:
Radon is a radioactive gas that you cannot see, smell, or taste. It forms in soil and rocks. People who work in mines may be exposed to radon. In some parts of the country, radon is found in houses. Radon damages lung cells, and people exposed to radon are at increased risk of lung cancer. The risk of lung cancer from radon is even higher for smokers.
* Asbestos and other substances:
People who have certain jobs (such as those who work in the construction and chemical industries) have an increased risk of lung cancer. Exposure to asbestos, arsenic, chromium, nickel, soot, tar, and other substances can cause lung cancer. The risk is highest for those with years of exposure. The risk of lung cancer from these substances is even higher for smokers.
* Air pollution:
Air pollution may slightly increase the risk of lung cancer. The risk from air pollution is higher for smokers.
* Family history of lung cancer:
People with a father, mother, brother, or sister who had lung cancer may be at slightly increased risk of the disease, even if they don't smoke.
* Personal history of lung cancer:
People who have had lung cancer are at increased risk of developing a second lung tumor.
* Age over 65:
Most people are older than 65 years when diagnosed with lung cancer.
Researchers have studied other possible risk factors. For example,
having certain lung diseases (such as tuberculosis or bronchitis) for
many years may increase the risk of lung cancer. It's not yet clear
whether having certain lung diseases is a risk factor for lung cancer.
People who think they may be at risk for developing lung cancer should
talk to their doctor. The doctor may be able to suggest ways to reduce
their risk and can plan an appropriate schedule for checkups. For people
who have been treated for lung cancer, it's important to have checkups
after treatment. The lung tumor may come back after treatment, or
another lung tumor may develop. Screening
Screening tests may help doctors find and treat cancer early. They have been shown to be very helpful in some cancers such as breast cancer. Currently, there is no generally accepted screening test for lung cancer. Several methods of detecting lung cancer have been studied as possible screening tests. The methods under study include tests of sputum (mucus brought up from the lungs by coughing), chest x-rays, or spiral (helical) CT scans. You can read more about these tests in the Diagnosis section. However, screening tests have risks. For example, an abnormal x-ray result could lead to other procedures (such as surgery to check for cancer cells), but a person with an abnormal test result might not have lung cancer. Studies so far have not shown that screening tests lower the number of deaths from lung cancer. You may want to talk with your doctor about your own risk factors and the possible benefits and harms of being screened for lung cancer. Like many other medical decisions, the decision to be screened is a personal one. Your decision may be easier after learning the pros and cons of screening.
Symptoms
Early lung cancer often does not cause symptoms. But as the cancer grows, common symptoms may include:
* a cough that gets worse or does not go away
* breathing trouble, such as shortness of breath
* constant chest pain
* coughing up blood
* a hoarse voice
* frequent lung infections, such as pneumonia
* feeling very tired all the time
* weight loss with no known cause Most often these symptoms are not due to cancer. Other health problems can cause some of these symptoms. Anyone with such symptoms should see a doctor to be diagnosed and treated as early as possible.
Diagnosis
If you have a symptom that suggests lung cancer, your doctor must find out whether it's from cancer or something else. Your doctor may ask about your personal and family medical history. Your doctor may order blood tests, and you may have one or more of the following tests:
* Physical exam:
Your doctor checks for general signs of health, listens to your breathing, and checks for fluid in the lungs. Your doctor may feel for swollen lymph nodes and a swollen liver.
* Chest x-ray:
X-ray pictures of your chest may show tumors or abnormal fluid.
* CT scan:
Doctors often use CT scans to take pictures of tissue inside the chest. An x-ray machine linked to a computer takes several pictures. For a spiral CT scan, the CT scanner rotates around you as you lie on a table. The table passes through the center of the scanner. The pictures may show a tumor, abnormal fluid, or swollen lymph nodes. Finding Lung Cancer Cells The only sure way to know if lung cancer is present is for a pathologist to check samples of cells or tissue. The pathologist studies the sample under a microscope and performs other tests. There are many ways to collect samples. Your doctor may order one or more of the following tests to collect samples
: * Sputum cytology:
Thick fluid (sputum) is coughed up from the lungs. The lab checks samples of sputum for cancer cells. * Thoracentesis:
The doctor uses a long needle to remove fluid (pleural fluid) from the chest. The lab checks the fluid for cancer cells.
* Bronchoscopy:
The doctor inserts a thin, lighted tube (a bronchoscope) through the nose or mouth into the lung. This allows an exam of the lungs and the air passages that lead to them. The doctor may take a sample of cells with a needle, brush, or other tool. The doctor also may wash the area with water to collect cells in the water.
* Fine-needle aspiration:
The doctor uses a thin needle to remove tissue or fluid from the lung or lymph node. Sometimes the doctor uses a CT scan or other imaging method to guide the needle to a lung tumor or lymph node.
* Thoracoscopy:
The surgeon makes several small incisions in your chest and back. The surgeon looks at the lungs and nearby tissues with a thin, lighted tube. If an abnormal area is seen, a biopsy to check for cancer cells may be needed.
* Thoracotomy:
The surgeon opens the chest with a long incision. Lymph nodes and other tissue may be removed.
* Mediastinoscopy:
The surgeon makes an incision at the top of the breastbone. A thin, lighted tube is used to see inside the chest. The surgeon may take tissue and lymph node samples.
You may want to ask these questions before the doctor takes a sample of tissue:
* Which procedure do you recommend? How will the tissue be removed?
* Will I have to stay in the hospital? If so, for how long?
* Will I have to do anything to prepare for it?
* How long will it take? Will I be awake? Will it hurt?
* Are there any risks? What is the chance that the procedure will make my lung collapse? What are the chances of infection or bleeding after the procedure?
* How long will it take me to recover? * How soon will I know the results? Who will explain them to me?
* If I do have cancer, who will talk to me about next steps? When?
Types of Lung Cancer
The pathologist checks the sputum, pleural fluid, tissue, or other samples for cancer cells. If cancer is found, the pathologist reports the type. The types of lung cancer are treated differently. The most common types are named for how the lung cancer cells look under a microscope:
* Small cell lung cancer:
About 13 percent of lung cancers are small cell lung cancers. This type tends to spread quickly.
* Non-small cell lung cancer:
Most lung cancers (about 87 percent) are non-small cell lung cancers. This type spreads more slowly than small cell lung cancer.
Staging To plan the best treatment, your doctor needs to know the type of lung cancer and the extent (stage) of the disease. Staging is a careful attempt to find out whether the cancer has spread, and if so, to what parts of the body. Lung cancer spreads most often to the lymph nodes, brain, bones, liver, and adrenal glands. When cancer spreads from its original place to another part of the body, the new tumor has the same kind of cancer cells and the same name as the original cancer. For example, if lung cancer spreads to the liver, the cancer cells in the liver are actually lung cancer cells. The disease is metastatic lung cancer, not liver cancer. For that reason, it's treated as lung cancer, not liver cancer. Doctors call the new tumor "distant" or metastatic disease.
Staging may involve blood tests and other tests:
* CT scan:
CT scans may show cancer that has spread to your liver, adrenal glands, brain, or other organs. You may receive contrast material by mouth and by injection into your arm or hand. The contrast material helps these tissues show up more clearly. If a tumor shows up on the CT scan, your doctor may order a biopsy to look for lung cancer cells.
* Bone scan:
A bone scan may show cancer that has spread to your bones. You receive an injection of a small amount of a radioactive substance. It travels through your blood and collects in your bones. A machine called a scanner detects and measures the radiation. The scanner makes pictures of your bones on a computer screen or on film.
* MRI:
Your doctor may order MRI pictures of your brain, bones, or other tissues. MRI uses a powerful magnet linked to a computer. It makes detailed pictures of tissue on a computer screen or film.
* PET scan:
Your doctor uses a PET scan to find cancer that has spread. You receive an injection of a small amount of radioactive sugar. A machine makes computerized pictures of the sugar being used by cells in the body. Cancer cells use sugar faster than normal cells, and areas with cancer look brighter on the pictures. Stages of Small Cell Lung Cancer Doctors describe small cell lung cancer using two stages:
* Limited stage:
Cancer is found only in one lung and its nearby tissues.
* Extensive stage:
Cancer is found in tissues of the chest outside of the lung in which it
began. Or cancer is found in distant organs. The treatment options are
different for limited and extensive stage small cell lung cancer. See
the Treatment section for information about treatment choices. Stages of
Non-Small Cell Lung Cancer Doctors describe non-small cell lung cancer
based on the size of the lung tumor and whether cancer has spread to the
lymph nodes or other tissues:* Occult stage:
Lung cancer cells are found in sputum or in a sample of water collected during bronchoscopy, but a tumor cannot be seen in the lung.
* Stage 0:
Cancer cells are found only in the innermost lining of the lung. The tumor has not grown through this lining. A Stage 0 tumor is also called carcinoma in situ. The tumor is not an invasive cancer.
* Stage IA:
The lung tumor is an invasive cancer. It has grown through the innermost lining of the lung into deeper lung tissue. The tumor is no more than 3 centimeters across (less than 1 ¼ inches). It is surrounded by normal tissue and the tumor does not invade the bronchus. Cancer cells are not found in nearby lymph nodes.
* Stage IB:
The tumor is larger or has grown deeper, but cancer cells are not found in nearby lymph nodes. The lung tumor is one of the following (see the picture of the main bronchus and pleura): -The tumor is more than 3 centimeters across. - It has grown into the main bronchus. - It has grown through the lung into the pleura.
* Stage IIA:
The lung tumor is no more than 3 centimeters across. Cancer cells are found in nearby lymph nodes.
* Stage IIB:
The tumor is one of the following:
-Cancer cells are not found in nearby lymph nodes, but the tumor has invaded the chest wall, diaphragm, pleura, main bronchus, or tissue that surrounds the heart
- Cancer cells are found in nearby lymph nodes, and one of the following:
*The tumor is more than 3 centimeters across
. * It has grown into the main bronchus.
* It has grown through the lung into the pleura.
* Stage IIIA:
The tumor may be any size. Cancer cells are found in the lymph nodes near the lungs and bronchi, and in the lymph nodes between the lungs but on the same side of the chest as the lung tumor.
* Stage IIIB:
The tumor may be any size. Cancer cells are found on the opposite side of the chest from the lung tumor or in the neck. The tumor may have invaded nearby organs, such as the heart, esophagus, or trachea. More than one malignant growth may be found within the same lobe of the lung. The doctor may find cancer cells in the pleural fluid.
* Stage IV:
Malignant growths may be found in more than one lobe of the same lung
or in the other lung. Or cancer cells may be found in other parts of the
body, such as the brain, adrenal gland, liver, or bone.
Treatment:
* Local therapy:Surgery and radiation therapy are local therapies. They remove or destroy cancer in the chest. When lung cancer has spread to other parts of the body, local therapy may be used to control the disease in those specific areas. For example, lung cancer that spreads to the brain may be controlled with radiation therapy to the head.
*Systemic therapy:
Chemotherapy and targeted therapy are systemic therapies. The drugs
enter the bloodstream and destroy or control cancer throughout the body.Second Opinion
Before starting treatment, you might want a second opinion about your diagnosis and treatment plan. Many insurance companies cover a second opinion if you or your doctor requests it. It may take some time and effort to gather your medical records and see another doctor. In most cases, a brief delay in starting treatment will not make treatment less effective. To make sure, you should discuss this delay with your doctor. Sometimes people with lung cancer need treatment right away. For example, a doctor may advise a person with small cell lung cancer not to delay treatment more than a week or two. There are many ways to find a doctor for a second opinion. You can ask your doctor, a local or state medical society, a nearby hospital, or a medical school for names of specialists. Also, your nearest cancer center can tell you about doctors who work there.
Comfort Care
Lung cancer and its treatment can lead to other health problems. You may need comfort care to prevent or control these problems. Comfort care is available both during and after treatment. It can improve your quality of life. Your health care team can tell you more about the following problems and how to control them:
* Pain:
Your doctor or a pain control specialist can suggest ways to relieve or reduce pain.
* Shortness of breath or trouble breathing:
People with lung cancer often have trouble breathing. Your doctor may refer you to a lung specialist or respiratory therapist. Some people are helped by oxygen therapy, photodynamic therapy, laser surgery, cryotherapy, or stents.
* Fluid in or around lungs:
Advanced cancer can cause fluid to collect in or around the lungs. The fluid can make it hard to breathe. Your health care team can remove fluid when it builds up. In some cases, a procedure can be done that may prevent fluid from building up again. Some people may need chest tubes to drain the fluid.
* Pneumonia:
You may have chest x-rays to check for lung infections. Your doctor can treat infections.
* Cancer that spreads to the brain:
Lung cancer can spread to the brain. The symptoms may include headache, seizures, trouble walking, and problems with balance. Medicine to relieve swelling, radiation therapy, or sometimes surgery can help. People with small cell lung cancer may receive radiation therapy to the brain to try to prevent brain tumors from forming. This is called prophylactic cranial irradiation
. * Cancer that spreads to the bone:
Lung cancer that spreads to the bone can be painful and can weaken bones. You can ask for pain medicine, and the doctor may suggest external radiation therapy. Your doctor also may give you drugs to help lower your risk of breaking a bone.
* Sadness and other feelings:
It's normal to feel sad, anxious, or confused after a diagnosis of a serious illness. Some people find it helpful to talk about their feelings.
Nutrition
It's
important for you to take care of yourself by eating well. You need the
right amount of calories to maintain a good weight. You also need enough
protein to keep up your strength. Eating well may help you feel better
and have more energy. Sometimes, especially during or soon after
treatment, you may not feel like eating. You may be uncomfortable or
tired. You may find that foods don't taste as good as they used to. In
addition, the side effects of treatment (such as poor appetite, nausea,
vomiting, or mouth sores) can make it hard to eat well. Your doctor, a
registered dietitian, or another health care provider can suggest ways
to deal with these problems. Sources of Support
Learning you have lung cancer can change your life and the lives of those close to you. These changes can be hard to handle. It's normal for you, your family, and your friends to have many different and sometimes confusing feelings. You may worry about caring for your family, keeping your job, or continuing daily activities. Concerns about treatments and managing side effects, hospital stays, and medical bills are also common. Because most people who get lung cancer were smokers, you may feel like doctors and other people assume that you are or were a smoker (even if you weren't). You may feel as though you're responsible for getting cancer (or that others blame you). It's normal for anyone coping with a serious illness to feel fear, guilt, anger, or sadness. It may help to share your feelings with family, friends, a member of your health care team, or another person with cancer. Here's where you can go for support:
* Doctors, nurses, and other members of your health care team can answer many of your questions.
* Social workers, counselors, or members of the clergy can be helpful if you want to talk about your feelings or concerns. Often, social workers can suggest resources for financial aid, transportation, home care, or emotional support.
* Support groups also can help. In these groups, patients or their family members meet with other patients or their families to share what they have learned about coping with the disease and the effects of treatment. Groups may offer support in person, over the telephone, or on the Internet. You may want to talk with a member of your health care team about finding a support group.